What is the Lymphatic System and why does Lymphoedema develop?
10th Dec 2020
If we have lymphoedema, or are at risk of developing lymphoedema, a better understanding of how our lymphatic system works will help us to understand why lymphoedema can develop when the system fails to work properly. Appreciating the function of the lymphatic system also makes us more aware of the importance of looking after our lymphatics and avoiding risks which may contribute towards lymphoedema developing or worsening.
The Lymphatic System
The lymphatic system is part of the body's immune system, having an important role to play in fighting harmful cells, for example, bacteria. It consists of lymph fluid, lymph nodes, lymph vessels and lymph tissue in a network of channels and glands throughout the body.
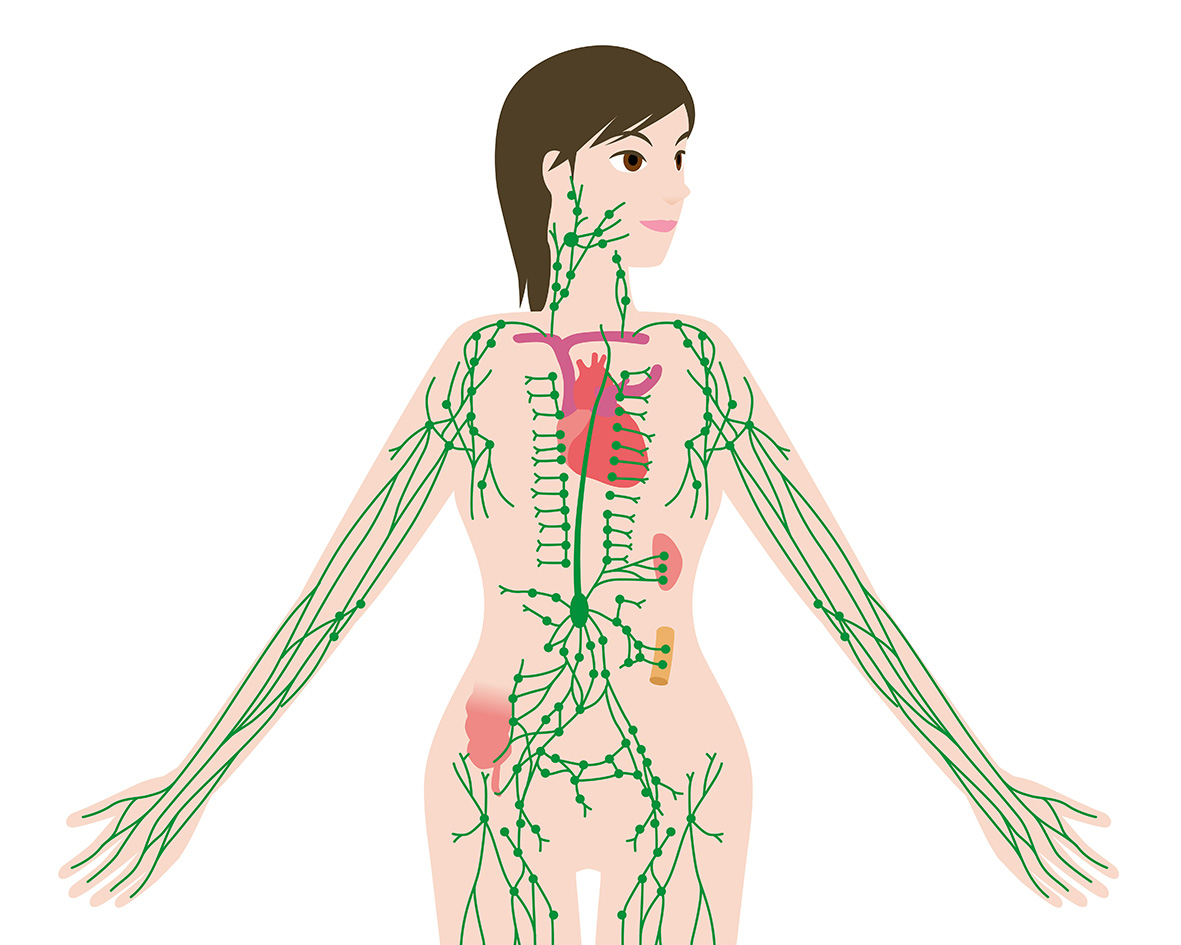
Although the lymphatic system is sometimes referred to as the body’s “second circulation”, it is in fact, a one-way drainage system and does not circulate in the same way as blood circulates. However, like our circulation, the lymphatic system works continuously; tiny blood vessels (capillaries) in the tissues just below the surface of the skin constantly leak water and protein, and this is drained away by another set of minute vessels called lymphatic capillaries. This protein rich fluid (lymph) then moves through the progressively larger, wider and deeper vessels of the lymphatic system and is eventually passed out as urine.
On its journey the lymph passes through lymph nodes, where it is filtered. We each have around 700 - 900 lymph nodes and these play an important part in immunology (fighting infection and inflammation), as well as digesting fat and maintaining fluid balance.
Adequate flow of lymph fluid is dependent on muscle contractions, breathing, and exercise and movement, and wearing a compression garment will enhance the action of the lymphatics.
Please see our blog posted on 26.02.2020 “An overview of Compression and its benefits”
Why does Lymphoedema develop?
If the lymphatics become blocked or damaged, water and protein cannot be drained away as normal, causing these to build up in the tissues and resulting in lymphoedema.
What is Lymphoedema?
What we often call Lymphoedema may fall into one of three different categories – Lymphoedema, Oedema or Chronic Oedema.
LYMPHOEDEMA
Results from a failure of the lymphatic system. It most commonly affects the lower or upper limbs, but the head and neck, trunk, breast or genitalia may also be affected. Lymphoedema may be Primary or Secondary.
Primary Lymphoedema
In Primary Lymphoedema there is an abnormality of the lymphatic system which is present from birth but may not become evident until later in life. This may happen if there is further damage to the lymphatic system, such as injury, infection, or trauma (such as surgery), which can upset fluid balance and cause the swelling to become noticeable.
Primary Lymphoedema may be hereditary, as in Milroy’s Disease, and work is currently ongoing into the many genetic causes of Primary Lymphoedema, with the hope that gene therapy may become available in the future for some people who have Primary Lymphoedema (BLS, 2020).
Secondary Lymphoedema
Secondary Lymphoedema is caused by damage to a normally functioning lymphatic system, and may be due to surgery, radiotherapy, trauma, or infection. For a few people lymphatics can be blocked by cancer, although lymphoedema which appears months or even years after successful treatment for cancer is usually due to local scarring and not to the disease itself.
OEDEMA
An imbalance of tissue fluid, caused when more fluid enters the tissues from the circulation than can effectively be drained away by the lymphatic system, such as in cardiac or renal disease. The system soon becomes overwhelmed and in time the oedema becomes chronic.
CHRONIC OEDEMA
Occurs due to an ongoing underlying problem which prevents the venous and lymphatic systems from maintaining fluid balance. Oedema is said to become chronic when it has been present for more than 3 months and no longer reduces with elevation of the limb(s). The causes include venous disease, trauma, infection, surgery, dependency and/or immobility, cardiac or renal insufficiency, and obesity (ILF, 2008).
Due to the lymphatic system failing to work normally in chronic oedema, the term “lymphoedema” may also be used.
The consequences of unmanaged lymphoedema or chronic oedema include :
- Swelling, which gradually increases over time.
- Changes in the skin, which becomes dry and may crack, with lymph blisters developing, giving a “warty” appearance to the skin’s surface.
- Changes in the tissues, with tissue fluid gradually replaced by fibrosis (scar tissue) and adipose or fatty tissue, which feels thicker and “spongy” or firmer to the touch.
- An increased risk of infection, or cellulitis, which in turn further damages the superficial lymphatics.
Appropriate treatment will help to minimise these common complications
Managing Lymphoedema
Lymphoedema is a chronic and a long-term condition as any damage to the lymphatic system cannot be reversed. But although your arm(s) or leg(s) will always have a tendency to swell, lymphoedema can be controlled. The management of lymphoedema encompasses a program of self-care, supported by your Lymphoedema Specialist Team, and involves skin care, exercise and movement, lymphatic drainage (massage) and wearing a compression sleeve or stocking. Unless your lymphoedema is mild you will probably always need to wear a sleeve or stocking in order to ensure the swelling is kept under control, and there are many acceptable styles and colour choices available from the Haddenham range of compression garments (www.hadhealth.com).
Continuing to maintain a healthy lifestyle and careful weight management are essential for a good outcome from any lymphoedema treatments, and it is always better if lymphoedema can be identified and treated early.
For more tips on self-care management please see our Blog posted 21 April 2020; “Looking after your lymphoedema”.
REFERENCES
British Lymphology Society (2020) BLS Lymph Facts: What is Lymphoedema? Available at: www.thebls.com
International Lymphoedema Framework (ILF) (2006) Best Practice for the management of lymphoedema: International consensus. London: MEP Ltd. 2006. Available from: